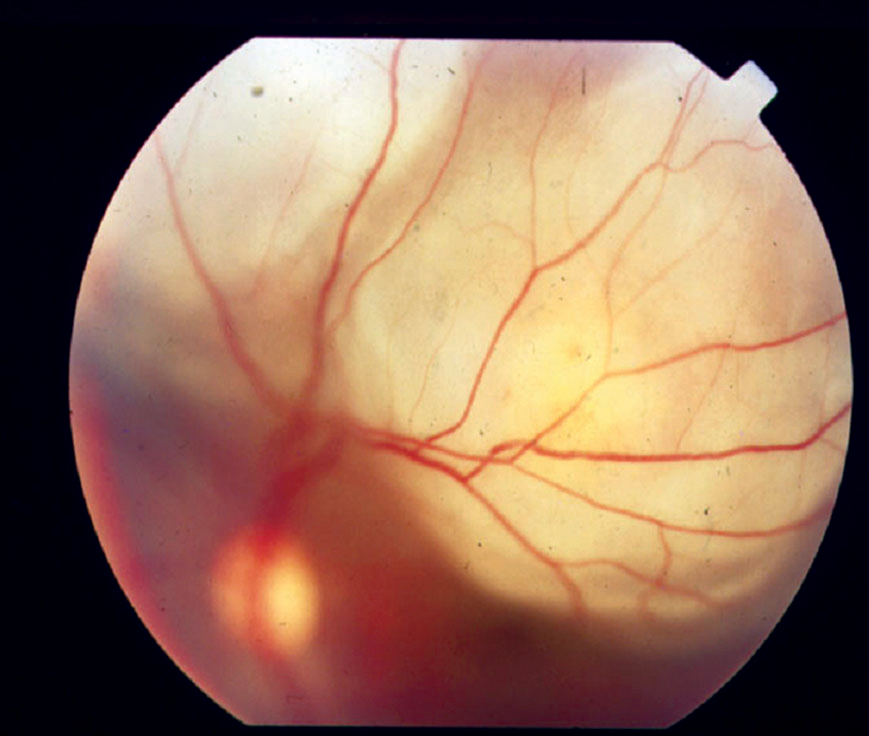
Sudden light sensitivity or a hazy veil over one eye can jolt anyone, hinting at uveitis—inflammation deep within the eye’s vascular layers. This condition strikes young and old alike, potentially scarring vision if unchecked. From clinic frontlines, I’ve seen patients dodge permanent blur through swift recognition and care. Grasping its triggers and tactics empowers proactive defense, safeguarding sight’s vibrancy.
The Anatomy of Uveitis Explained
Uvea houses iris, ciliary body, choroid—rich in blood vessels prone to immune fury. Anterior hits front chambers with pain; posterior clouds back vision subtly. Panuveitis engulfs all, rare but fierce.
Idiopathic cases dominate, but infections, autoimmune flares, or toxins lurk. Symptoms vary: redness without itch, floaters multiplying overnight. Awareness accelerates intervention.
Distinguishing Types by Location
Slit-lamp exams pinpoint zones; OCT scans depth precisely. Juvenile idiopathic arthritis often pairs with anterior. Patterns guide therapies uniquely.
Spotting Early Warning Signs
Photophobia forces squinting indoors; blurred near vision persists despite glasses. Pupil irregularities or vitreous haze emerge on dilation. Pain throbs dully, worsening touch.
Fever or joint aches signal systemic roots. Log episodes—patterns reveal recurrences. Prompt logs save acuity.
AllAboutVision details ocular synechia risks from adhesions in uveitis, stressing vigilance.
Risk Factors You Can Influence
Smoking ignites flares; stress amplifies autoimmunity. Toxoplasmosis from undercooked meat lurks. Hygiene curbs infections tying to eyes.
Diagnostic Tools in Modern Practice
Fluorescein angiography lights vessel leaks; B-scans ultrasound haze. Bloodwork hunts HLA-B27 or Lyme markers. OCT quantifies macular edema swelling.
Targeted imaging trims guesswork. Results shape attacks precisely.
Healthcare coalitions debate access, as coverage jockeying in Medi-Cal spending eyes ballot initiatives, impacting timely uveitis diagnostics for many.
Treatment Strategies That Work
Corticosteroid drops taper inflammation hourly at peaks; implants sustain back-of-eye delivery. Immunosuppressants like methotrexate quiet systemic storms. Biologics target TNF for recalcitrant cases.
Antibiotics pair for infections; antivirals fend herpes kin. Tailoring blends potency with minimal sides. Monitoring adjusts dynamically.
For persistent threats demanding precision, Eye Surgery Today covers vitrectomy or lasers breaking synechiae effectively.
Managing Side Effects Proactively
Drops raise pressures—beta-blockers counter. Steroid cataracts? Surgery clears post-stabilization. Weigh benefits against watches.
Preventing Recurrences Through Lifestyle
Sunglasses shield flares; omega-3s dampen cytokines. Vaccinations block triggers like flu. Stress logs prompt mindfulness pauses.
Regular rheumatology syncs catch brewing storms. Diet shuns processed igniters. Habits forge stability.
Role of Regular Monitoring
Quarterly dilations track quiet smolders. Visual fields map subtle losses. Data drives preemption.
When Uveitis Demands Specialist Care
Macular involvement threatens reading; optic nerve hits fields asymmetrically. Pediatric uveitis risks amblyopia—multispecialty teams excel. Referrals preserve potentials.
Trials test JAK inhibitors promisingly. Horizons brighten.
Patient Education Empowers
Apps log symptoms; flare kits stock drops. Knowledge curbs panic. Partners thrive informed.
Voices from Recovery
Teacher Elena’s anterior flares halted school vision; drops restored chalkboard clarity. Artist Kai battled posterior haze—biologics revived palettes. Golfer Pat sidestepped panuveitis scars via vaccines. Triumphs underscore speed.
Setbacks teach resilience; adjusted meds rebound stronger.
Conclusion
Uveitis demands swift diagnostics, layered treatments, and vigilant prevention to shield delicate uvea layers. From drops to lifestyles, integrated approaches tame flares durably. Heed signals, partner with pros, and sustain the sharp, pain-free gaze uveitis once clouded.
